1 in 5 Americans suffer from chronic pain, as per the CDC. When dealing with chronic pain, many patients are prescribed opiates. Unfortunately, most opiates are highly addictive. According to a study by the Center for Disease and Control CDC, an opioid prescription that lasted for over eight days increased the likelihood of drug use by 13.5% a year later [1]. For a prescription of 31 days, the chances of long-term opioid use increased to 29.9%.
Opiate addiction is becoming much more common than most people want to believe. After getting hooked on opiates and opioids, it’s difficult to get clean, and sobriety may feel unattainable. However, there’s always a way forward. In addition to seeking opioid addiction treatment from a rehab facility, you can learn how to manage pain in your life with non opioid pain control. By managing pain and finding different ways to deal with it, you can completely break opiate dependence.
Avenues Recovery has treated countless opioid users all the way through to sobriety. We know that when opioid use starts for pain relief, addiction can be quick to follow. Our clinical professionals practice many alternative pain relief options. Read on to hear their top 9 recommendations on how to relieve pain without medicine.
#1. Exercise: The Ultimate Non Opioid Pain Control
Scientists have known for a long time that exercise can reduce pain, and therefore provides a non opioid pain management option. A recent study [2] measuring the pain tolerance of patients discovered that patients who exercised regularly as part of their different treatment programs had a higher pain tolerance than those who didn’t. They could withstand more pain although their pain thresholds had not actually changed.
When exercising, the body releases several natural opiates, such as endorphins. These endorphins attach to receptors in the brain to reduce pain and dampen discomfort. This effect is known as exercise-induced hypoalgesia. It lasts for about 20 to 30 minutes after the workout.

There are several different types of exercises that can help with pain management. They include:
- Range-of-motion exercises
These types of exercises relieve stiffness and increase mobility around the joints. Most of these exercises are rather simple - they involve easy movements like rolling the shoulders forward and backward. - Strengthening exercises
These types of exercises help to build stronger muscles. Common exercises include bench pressing and weightlifting. It’s best to avoid working out the same muscle groups two days in a row. - Aerobic exercises
These types of exercises improve your cardiovascular health, as well as general health. They include walking, biking and even swimming.
Other activities, no matter how small, can also help to reduce pain. Some people might go for just a quick walk or jog around the block. Others may rake leaves or even mow the lawn. Many treatment facilities incorporate some type of activity or exercise into their routine. Those with opioid use disorders will benefit from producing more natural opiates instead of relying on artificial products, making exercise a natural top choice for non opiate pain control.
#2. Relax Via Deep Breathing or Meditation

Meditation and deep breathing calm the mind while recharging the body. Both meditation and deep breathing help to lessen tension in the muscles. Tight muscles increase pressure on the nerves and receptors, which can increase pain. By relaxing through deep breathing and meditation, the pain-tension cycle breaks.
These techniques are particularly helpful in improving one’s mental health. Many rehab facilities offer yoga sessions and meditation rooms for addicts, especially those with a prescription opioid addiction.
Deep breathing is another great option for non opioid pain management. It’s also one of the easiest skills to practice. It involves taking deep breaths to lessen muscle tension. Shallow, rapid breathing is believed to cause tension.
If you are interested in learning a deep breathing technique, we recommend you find a quiet and warm space. Breathe deeply through your nose or mouth and relax your stomach muscles. Take deep, slow breaths at your own pace. When breathing out, picture tension leaving your body. This technique is great for dealing with the withdrawal symptoms involved with opiate addiction.
#3. Look For Ways to Release Stress

Did you know that negative feelings, like depression and stress, can increase your body’s sensitivity to pain? The more stressed you feel, the more sensitive to pain you become. Learning how to take control of stress is quite possibly one of the most effective alternative methods of pain relief. There are many different types of techniques that you can use to reduce stress. Try spending time doing hobbies and relaxing activities. Some of the most recommended techniques include:
- Listening to relaxing and soothing music
- Using mental imagery for a mental escape
- Relaxing with progressive muscle relaxation
Relieving stress relaxes the muscles. This puts less pressure on pain receptors in the body. In addition, less stress results in the more natural production of neurotransmitters responsible for creating feelings of euphoria. People who are less stressed are more likely to feel happy and pain-free. They are also less likely to reuse opioids or be at risk for an opioid overdose.
#4. Switch to a Healthier Diet
Want to know how to relieve pain without pills? Your diet can make a world of a difference when it comes to alternative methods of pain relief. You are what you eat. Many nutritionists recommend including natural painkillers in your diet. This is an easy way to manage pain without using conventional analgesics. The main types of natural painkillers to look for include:
- Curcumin [3] is found in turmeric and works as an anti-inflammatory drug.
- Quercetin is found in red onions, red wine, and citrus fruits. This natural compound inhibits inflammation.
- Omega-3 fats are found in salmon and walnuts.

The real magic happens when all of these natural compounds are taken together at the same time. It’s important to have a good amount of all of the above in your diet to help ease pain. Additionally, these compounds also have other health benefits. For example, curcumin prevents cognitive decline that’s associated with aging keeping your mind healthy and active.
Eating healthily is hugely beneficial for non opioid pain management. This includes eating natural products and shying away from processed foods. Those who are more unhealthy are more likely to experience other health conditions that might exacerbate the pain. It’s vital to find a treatment program that offers healthy dining options, in order to give you the best chance at recovery.
#5. Acupuncture

The National Institute for Health and Clinical Excellence recommends acupuncture as an alternative pain relief. There are different approaches and schools to acupuncture. The different schools target pain relief in different ways.
The Eastern school attempts to balance the body’s flow of yin and yang energy. Fine needles are inserted into specific acupressure points in the body. The Western approach, on the other hand, inserts a needle directly into the center of the affected area. Both approaches are effective and can help manage pain.
Inserting acupuncture needles into the body stimulates the central nervous system. This diffuses pain signals in the brain and dulls pain. The insertion of a needle also stimulates blood flow to the area. Increased blood flow reduces inflammation, eases muscle spasms, and stimulates endorphin production. Endorphins are one of the body’s natural painkillers which help to ease pain naturally. An increase in endorphins is particularly beneficial for opioid addicts seeking sobriety alongside pain relief.
There have been many cases where acupuncture has successfully offered pain relief. Recent studies have explored the positive correlation between chronic lower back pain relief and acupuncture. Acupuncture not only treats pain but also improves function in that area of the body.
Several acupuncture sessions may be needed before an effect is felt. You may also need ongoing acupuncture to help ease and manage pain. If you’re afraid of needles, another option to try is acupressure, which works in a similar way to acupuncture. Acupressure is great for treating alcohol dependence and drug dependence As it works by easing any withdrawal syndrome associated with addiction. Opioid withdrawal symptoms can be particularly difficult to overcome.
#6. Hanna Somatics

The Hanna Somatics [4] is an interesting mind-body technique created by Dr. Thomas Hanna in the 1970s. This neuromuscular movement re-education is highly effective. It also treats the root cause of most chronic muscular pain. This way, opiates are not needed anymore.
The heart of this therapy functions under the belief that the brain is the control center for muscles. As a result, those who learn how to control the brain can indirectly control their muscles or nerves. Drug addicts who are practicing the techniques in Hanna Somatics will be guided through several slow, mindful movements. These movements increase awareness of tension and movement in the body. It helps the brain learn how to sense and organize muscle movement. They learn how to regain awareness and sensation in the motor control of muscles via an educational process. This leads to improved muscle function and enhanced sensory awareness. Surprisingly, this is a great way to ease pain and manage stress.
This technique targets sensory motor amnesia (SMA). It can not only relieve pain but also deal with:
- Headaches
- Stiff or painful muscles and joints
- Fatigue
- Poor posture
- Back pain
- Repetitive use injuries, or stress injuries
The technique is easy to learn and quick to pick up, with many classes available which teach it. This therapy is particularly popular with opioid users and drug abusers. Constant stimulation of the opioid receptors may have caused some connections to become wonky and Hanna Somatics can completely reteach the brain how to function.
#7. Hypnosis

Substance abuse and mental health problems often come hand in hand. The treatment of opioid dependence should include improving mental connections in the brain. Hypnosis is believed to be one of the effective non opioid pain alternatives. In fact, a study conducted at Harvard found that hypnosis was even effective in reducing pain from surgery. This technique works by refocusing the mind away from pain.
Several sessions may be needed for hypnosis to work. This type of maintenance treatment can help patients learn how to diminish their focus on pain. Hypnosis can also be used as a treatment for opioid addiction. It can be especially helpful for patients with high drug tolerance.
#8. Get an Injection of Your Own Blood
Although it doesn’t sound appealing, getting an injection of your own blood can help treat pain and acts as an excellent non opioid pain control. In fact, this technique is known as platelet-rich plasma therapy (PRP), and it’s been successfully used to treat a variety of medical conditions in the US for decades.
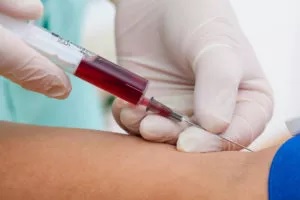
How Does Platelet-rich Plasma Therapy Treatment Work?
Platelets stimulate a healing cascade in the body. When injected back into the body, it will stimulate cells and cause them to start to repair any damaged tissues that are nearby. This causes a rush of certain neurotransmitters that can also help reset the brain. The entire process enables patients to feel more at ease and helps many drug abusers deal with their addiction to opioids and opiates.
If you’re interested in this type of treatment, make sure that you get it from professional healthcare providers. It’s also important to let the healthcare providers know if you are taking any prescription pain medications at the time. If you are taking any prescription medicines, you may not be able to try this treatment out. PRP is recommended as a maintenance treatment for staying off of prescription pain medications and other drugs and alcohol.
#9. Find and Join A Support Group

A huge part of pain is emotional. Learning the skills to handle emotions will make any sobriety journey easier. Therapy and support groups do wonders in easing psychological symptoms. Psychological dependence is equally as hard to break free from. Your body may no longer crave the drug, but your mind does. There are plenty of support groups to choose from. Some of the most popular options include:
- Cognitive Behavioral Therapy (CBT)
- 12 Step programs
- Family counseling
- Group counseling
- One-on-one counseling
- Motivational Interviewing
Therapies can target different signs and symptoms of addiction. They can teach you how to identify triggers and build better habits. They can also help correct substance abuse and mental health issues. Most therapies teach different techniques for the management of opioid abuse. Addiction to opioids can be particularly difficult to recover from, however, there are many support groups available for those who are attempting to wean off of pain medications.
Non Opioid Pain Control is a Viable Option
It’s not easy to recover from opioid addiction. Even with professional help, users struggle. If you’re interested in learning how to get rid of your dependence on opioids, it’s time to learn alternative methods of pain relief.
Many rehab facilities will include different ways to break free from opiate addiction within their treatment of opioid abuse. Patients need to learn how to relieve their pain without pills that carry an addiction risk. It’s time to stop relying on prescription drugs and opiates. Instead, learn how to rely on yourself and get treatment for opioid addiction.
No matter where you stand in your recovery journey, Avenues Recovery is here to support you. If you’re seeking advice on non opioid pain management or looking to quit opioids altogether, our addiction treatment services can guide you all the way through. Contact us 24/7. You deserve a pain-free life.
Sources
[1] www.cdc.gov


